Jun 30, 2007
Thank You
Still, that's a LOT of hits, and I'm very impressed. Thanks!
On Superstition
I've never been a superstitious person....just the opposite. I don't like the idea of superstition, or luck, or anything similar, and I get particularly peeved when something happens to reinforce somebody else's superstition. It's like reinforcing a negative stereotype....it's harder to overcome preconceptions when they've just been supported "in the wild."
Two weeks ago, the day after Andrew was born, I jokingly said that I was going on a "shaving strike," and that I wouldn't shave again until Andrew came home from the hospital. It was mostly done as an excuse to ignore my razor for a few days, and to be funny, because I knew what D's response would be. I actually stuck to it for quite a while....Drew didn't seem to mind, since I couldn't touch him with my face anyway....but let's just say that other members of the household weren't as thrilled. I told Drew what I had said and warned him that I was going to shave, but that it meant he had turned a corner and was on the home stretch, getting better so that we could take him home. I ended up shaving on Thursday.
Now, it's Saturday, and he hasn't had a really GOOD day since I shaved. I know the two are completely mutually exclusive and have nothing to do with each other. I would argue that point forever. But it still annoys me that even the appearance of superstition has been reinforced, and I'm counting on Drew to prove this silly thing wrong.
Jun 29, 2007
A Frustrating Day
No need to call, email, or be concerned. It's just one day in a long series, and we all deserve to be Debbie Downer at some point. Days like this remind us how nice it is when he's doing well, and make us appreciate the doctors and nurses that have the patience to continue his care through any speed bumps.
On a positive note, his feedings are going better. As of last night, they had given up for a while, because he ended up with EVERYTHING he had eaten (and more) back in his stomach. They tried again while we were there today, but with a different strategy. Instead of giving him 5 cc's, they gave him 10, thinking that perhaps stretching his stomach out a bit would stimulate his digestive system. When they went back in (with a suction) to check for "residuals," it was less than 1 cc. They then gave him 10 more, which he also dealt with well. At 8pm he took another 10 and only gave back 2 in residual. Assuming he continues to do well, they'll repeat the pattern throughout the night.
Down Day
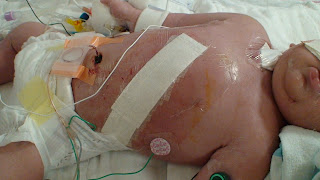
Everything else has been pretty stable. The surgeon came by and took off the tape and gauze on his chest, leaving only steri-strips over the scar. That relieved some of the redness on his chest, which may have been due to tightness from the tape. The steri-strips were re-taped, and his chest now looks better.
It looks like the feeding process will probably take a while. They've been trying to feed him for about 15 hours. They put a specific amount (5cc's for example) into his NG tube, which deposits it directly into his stomach. Three hours later, they use a syringe to extract whatever is left, so they can see how much is being digested. After the first feeding, there were 2.5 cc's left. They put it back, along with 2.5 more. The next time they suctioned, they retrieved 9 cc's (5 + 2.5 + 1.5 of other stuff). Like I said....long process. His stomach hasn't had to function correctly for two weeks, and now it needs some practice before it will work correctly. They'll try this out for a week or two before considering surgical options.
One final note....at the moment, Andrew looks a bit like a space alien. His cute little face looks just beautiful, but his head is very swollen with fluid. Moving his head around causes the fluid to move from one side to the other, but we'll have to be patient while his body actually processes (and discards through his urine) all the extra liquid. The last couple of days have been good for that....his urine output was higher than his fluid input, but it seems like it's all in his head. My cute little alien.
Jun 28, 2007
Jewelry Plans
When a child is taken off ECMO, the arteries and veins that were used (the carotid and jugular) are tied off and left as-is. There apparently has been no evidence that reattaching these vessels helps in any way, and prolonging the surgery to do the anastomosis (fancy medical term) is more dangerous because the blood is still a bit heparinized. This means that the major artery and vein connecting the heart to and from the brain on Andrew's left side are no longer functional. The vessels on the left side and the other (more minor) vessels on both sides will pick up the slack and shouldn't cause a problem, but it does mean that Andrew will have to wear a bracelet or necklace for the rest of his life.
MedicAlert notifications are oval-shaped medallions on a chain around a wrist or neck (bracelet or necklace) that provide notice to medical personnel of any existing condition of which they should be aware. People with diabetes, missing/transplanted organs, blood conditions, allergies, and other conditions wear these bracelets at all times. The medallions have the Staff of Aesculapius (snake winding around a staff) on one side and medical ID information on the other side. Andrew's will have to say that he has a severed carotid artery, as one of the signs of clinical death (to an EMT) is lack of a carotid pulse. We don't want anyone to 1) misdiagnose anything due to an unresponsive pulse, or 2) do anything to block his other carotid.
He doesn't have to get the bracelet right away, as we would normally be there to give instructions to any medical personnel. But as soon as he is out of the house on his own, at school or a friend's house, he'll need to get the tag. Maybe we'll get him some bling....a platinum version, perhaps?
Possible Future Surgeries
1) Stomach valve to reduce GERD (gastroesophageal reflux disease). Children with diaphragmatic hernias often have trouble eating post-operatively. This is because the diaphragm has a large role in keeping food going in the right direction. When food travels through the esophagus and down into the stomach, the diaphragm constricts so that the food is less likely to come back up. Since Andrew had very little diaphragm around his esophagus (though there was SOME), he may have this issue. The surgeon would go in and use his upper stomach to create a one-way valve to keep food in and prevent leakage.
2) Ladd procedure to reverse malrotation. When the intestines don't develop normally and in the correct place, they can't attach to the abdominal wall at the correct point, and often twist (malrotation). This twisting can cause a blockage, or allow "Ladd's bands" to form between the stomach and the small intestine. These are bands of tissue that keep food from traveling normally from the stomach to the intestine. During a surgery to correct these issues, the Ladd's bands are fixed and the large and small intestines are placed in the right location. During the hernia surgery, the focus was on getting everything removed from the chest cavity and closing him up before there was a problem with bleeding....mostly because of the ECMO. We'll have to wait and see how eating goes before we know if he needs either of these first two surgeries.
3) Diaphragm patch replacement. As I mentioned before, he may need to have the patch replaced later in life, most likely during puberty or near another major growth spurt. He has plenty of extra patch for years of initial growth.
None of these surgeries are anywhere near as major as the first, and none would have the additional complication of Andrew being on ECMO. How he responds to food in his digestive system will give us a better idea of his needs. I'll also talk to the surgeon about how he left the abdominal organs when he closed Andrew up the other day. It might give him an idea about percentage possibilities.
Like the Paula Abdul Song
As of last night, they were down to 32 on the vent....as of this morning, they had come down to 30 and then back up to 31. They've also brought the nitric oxide down to 2.5%. They'll decide tomorrow whether to continue with a slow wean or turn it off entirely. The other fun news is that they started feeding him this morning! They put in a new NG (nasogastric, from his nose to his stomach) tube this morning and gave him a tiny bit of food, just to see how he'll respond. If he does well, they'll continue....if he doesn't, they'll stick to the IV method for a bit.
We haven't talked to a doctor in a couple of days, but it seems like he's doing really well and making good progress. His oxygenation has been consistently good, and it's just a matter of getting his carbon dioxide down (that's what the hi-fi vent is helping with). I'll let the doctor make any predictions, but I'm definitely positive about the way things are going.
Jun 27, 2007
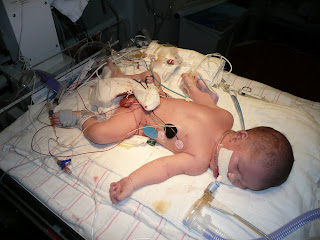
Post-ECMO Pictures
More Pictures Later
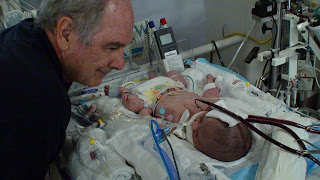
Daddy/Baby Comparison
War Wounds
Andrew may have to have more surgeries later....I think the 'probable' count is now up to three, but the ones he's already been through are the most critical. After healing and growing, his body will be able to handle them much more easily.
Besides, chicks dig scars.
Scared of the dark
Yesterday they were able to turn the amplitude (strength) on the hi-fi vent back to 34 (from 36), they turned the nitric oxide percentage down from 20 to 10, and they turned the oxygen percentage down from 53 to 46. All really good signs, though the nitrix oxide number is a bit misleading...even though they cut it in half in one day, they aren't going to be able to wean him completely for a long time.
However, last night his blood gas levels weren't quite as good, so they had to turn the vent back up to 36. The other two levels stayed the same, but he also needed some extra blood (for a low hematocrit level)....not a big deal. This morning his numbers were borderline, so they aren't going to try and come down any more for a little while. They'll probably reconsider tonight.
Jun 26, 2007
Diaphragm Update
Realistically, what this means is that some day he'll have to have the patch replaced. It won't be now, it won't be in the next few years, but at some point it will almost certainly require replacement. They'll keep an eye on him through major growth spurts (puberty, etc), as that time would be the most likely for a new herniation. Whether they would go in and replace it proactively or wait until he has another problem (MUCH more minor and treatable at that point), I'm not sure. The surgeon made the patch he put in very dome-shaped, meaning that he has a lot of extra material that can flatten out and "grow" with his body. It should last many years because of that "extra" area, and it will also show up on a chest X-ray when it begins to flatten out and get tighter.
I'm very confident with the meticulous work of the surgeon (who also suggested his scars would be relatively minor (long, but minor), and I think this solution will be effective for a long time. Baby's bodies are very resilient, and his other muscles will compensate for the lack of a diaphragm when breathing. He also has a full diaphragm on the right side, to go with his full lung, which will hopefully prove itself to be strong and useful in the next few weeks.
The other good news is that his left lung looks better than they were expecting. Instead of a nubbin or no lung at all, his lung is almost half-size. It has also formed two developed lobes instead of being stunted early, so it's not bad, just small. It should be able to expand, grow, develop, and fill a good portion of his left side (perhaps 3/4 of the cavity). That bodes well for his future lung volume.
Off ECMO and Stable
There are a few numbers they're generally looking at when deciding what to tweak. The first is his overall oxygen saturation, which represents how well his lungs are taking oxygen out of the air (or from the vent) and putting it into his bloodstream. If this number went down, they would have to turn up the percentage of oxygen in his vent (currently 50%).
The next is the difference in saturation between his upper body and lower body. If there's a big difference, it means the blood pressure around the heart/lung is too high and the blood isn't being oxygenated before traveling to the rest of the body. The solution to this problem is the inhaled nitric oxide, which helps dilate the nearby blood vessels and even out the pressure. Yesterday during the test off ECMO, they added the NO tank and his numbers immediately equalized.
The last is his carbon dioxide saturation. His lungs are supposed to take oxygen out of the air and stick it into his bloodstream, then take returning blood and pull out the carbon dioxide for exhalation. The better this process works, the lower the CO2 content in his blood, which reduces his blood acidity (a good thing). They will try to get to a stable number for Andrew, even if that number is a bit higher than a normal baby. Last night, his number was in the 70's, which led them to turn up the hi-fi vent strength. The high frequency vent has the effect of getting air into the lungs air sacs more efficiently, allowing for better gas exchange. By going up on the strength, they got his CO2 stable in the 50's.
Too much medical jargon, I know, but this is what we'll be living with for a while....it's just a matter of letting Andrew's body heal, his lungs develop, and his problems subside. When all his numbers look perfect on 30-40% oxygen, on a standard ventilator, with no nitric oxide, that's when they'll start thinking about letting him try to breathe on his own (I think). If you take anything away from this post, let it be this....his hernia has been fixed, the ECMO has been removed, and he is stable and healing. We've crossed a major hurdle.
Jun 25, 2007
Still Waiting
Thumbs Up
1) We are very tired...it was an early morning and we didn't sleep a lot last night.
2) There's still one surgery left to go. We were excited by the potential of doing it all at once, and it just extends the day (and the tension).
3) It's going to be a long road. He'll be on a ventilator for weeks to months...some severe cases are here for a year and a half. We are confident he won't be one of those cases, but even the best case will require a lot of patience and strength.
Surgery Details
Drew's surgery took a few hours (if not more) to complete. The reason is that there was very little diaphragm remaining on which to attach the patch. The surgeon had to rush off to another procedure, but the other attending doctor said that there was only a rim of muscle available around the edge of the abdominal cavity. The hernia also went from his left side all the way to his midline.
The downside to having so little to work with is that the diaphragm won't work on his left side for a long time, if ever. The muscle should stretch and make up for some of the slack later in life, but there's no guarantee. There's also a higher risk of a repeated hernia, though if it happened again it would be relatively minor (he would probably notice some trouble breathing) and would be a pretty simple fix. If it happened, it wouldn't be until later in life, so it'll just have to be something we keep in the back of our minds.
The organs included in the hernia were the stomach, intestines, a bit of liver, and a bit of spleen. There was a little bleeding from the spleen initially, but they quickly got it under control. There was no bleeding (to speak of) from the incision, the liver, or other organs. They were able to get all the organs down into the abdomen without any trouble, and they haven't seen anything in the way of surgery complications.
They took a chest X-ray after the surgery and saw a good amount of left lung...a little more than a third of his chest cavity on that side. It will take a while to determine the state of development and/or growth of that bit, but it's certainly more than the nubbin it could have been.
As I mentioned, he's still on ECMO for a few hours. They'll do another trial to see how he responds sometime this afternoon. That will tell them what sort of support he'll need from the ventilator. The options that can be modified are: percent of oxygen, nitric oxide (or not), and high frequency vent (or not). I'm guessing there's a 70% chance he'll need the hi-fi vent, but the hope is that he'll have some cushion room so there's a fall-back instead of ECMO.
We just saw him again and he still looks good. He'll be sedated for a full day to make sure he doesn't hurt himself, but I'll be sure to get pictures after the ECMO comes off. I'll post another update after the next surgery.
"Going well....almost done"
Morning Update
They kicked us out for the shift change, but we'll get to see him one more time before he moves to the OR. It's already 7:20 and they don't seem to be anywhere near starting, so I'd call this the first of several delays.
Jun 24, 2007
Last post for the night
All the nurses and doctors I've talked to in the last day sound VERY positive about his numbers and his responses to the challenges they've put forward. His lung(s) are responding nicely and they are confident that he will be able to handle being taken off the ECMO. Even at a flow of 12, they still haven't had to dial up the oxygen on his ventilator from 40%, so they have plenty of breathing room (no pun intended) if he needs additional support after surgery. We have the knowledge of hundreds of years of combined doctor/nurse experience taking care of our baby....some of the best in the country....and I feel confident that they'll do exactly what's best for Andrew.
Again, don't be alarmed if you don't hear from us for a while tomorrow. I'll try to post while we're waiting, but it could take a long time....and that doesn't have ANY bearing on the successful outcome.
Surgery Plans
They will turn his flow down by 1 step every hour until he's at 5. If he needs additional vent support, they'll turn it up, but he's been responding great so far without any need. When he gets to 5, they'll clamp the tubes in his neck for an hour and take blood gases every fifteen minutes. If everything is still good, they'll unclamp and turn the ECMO back up to 20, just to keep everything heparinized and flowing well through the machine. They'll do that twice through the night, which will reassure them of his stability without ECMO.
Assuming everything goes well, they'll do the surgery tomorrow morning at 7:30am. It will be a LONG process. First, they have to move him (and the ECMO) down the hall into the OR. Then they'll perform the actual surgery, during which they need to be very careful to clot (cauterize) every little capillary to prevent bleeding. The surgeon also does a lot of pediatric plastic surgery, so he is very precise and does a meticulous "close." When the hernia surgery is finished, they'll almost immediately remove the ECMO....they're pleased enough with his progress that they don't think he'll need it for long. Then they have to move him back to the NICU, and it'll be another half-hour before we get to go in and see him. Someone quoted 5 hours, but I would expect the total time to be more like seven or eight, so don't get worried if there are no quick updates.
There will be a lot of hurdles to overcome after the surgery, and it will be a long, hard process, but making it through the surgery tomorrow will be a huge milestone. There are many dangers inherent to the surgery itself, the additional clotting issues introduced by the ECMO, and the trauma of this pair of procedures on such a tiny body (not that 9 pounds is anything to sniff at). Though we are both nervous about the surgery, we are hopeful that it will put him in a very good place.
Update
We're waiting for D's mom and then we're going to head down and see him. Depending on his level of sedation, I'll try and get some more pictures.
Jun 23, 2007
On Morphine
When he gets too active, the nurses have to give him Ativan and/or morphine, which puts him to sleep pretty quickly. There's a fine line between "OK movement" and "too much movement," and though I tell him to be calm so they don't have to drug him, he's not the most well-behaved baby. I had to scold him the other day. :)
Right now he's sleeping because he was trying to play soccer and they had to drug him.
Update
He got an "oxy challenge" this morning, which is a test to see how well he'll respond to oxygen in his lungs. They turn up the ventilator to 100% and check the oxygen saturation in his blood....if it goes up, that means his body knows what to do with the oxygen and that he will probably respond well after coming off the ECMO. The results: his numbers went from fifty-something to over three hundred....a very positive sign.
Jun 22, 2007
Still Sick
As much as it pains me to miss an entire day at Andrew's bedside, it is definitely in his best interest. We'll be headed there early tomorrow morning....hopefully we'll both feel 100% better.
Logistics
I want to thank everyone again for the outpouring of love. Between our family, friends, and coworkers, we are very lucky to have such a wonderful support system. We've got four different sets of flowers, including a really neat potted gardenia, our refrigerator and freezer are filled with food brought by friends and family, our answering machine and voicemail are filled with warm messages (sorry for not answering), and my email inbox is overflowing with best wishes.
June 22, 2007 - Day 8
On the positive side, his flow is down to 25 and he's sounding very stable. The surgeon stopped by today and is shooting for a Monday surgery, though that's still very flexible.
Day 7 Pictures
June 21, 2007 - Day 7
His flow got down to 30 over the course of the day, and the doctors came up with a 'new plan' moving forward. Instead of turning up the ventilator and making him use his lungs more quickly, they have decided on a somewhat less aggressive approach. They plan to let him relax through the weekend, slowly bring down the ECMO flow, and then shoot for the surgery early next week. However, in order to do the surgery, he has to show them that he'll be able to survive off the ECMO, which means getting his flow down around 5.
We spoke with the surgeon, who made us feel pretty good about the surgery itself. As long as he can get stable before the surgery starts, I'm convinced that he'll be able to pull through afterwards. The surgery involves a rather large incision on his left side, just below the diaphragm. They'll open him up and carefully pull his abdominal organs down through the hole, then patch the hole with a sheet of Gore-Tex. If the hole is small enough, they might even be able to sew his diaphragm closed without the patch, but I don't have high hopes for that. As he grows, the patch will become a smaller and smaller percentage of his diaphragm, so it will never need to be replaced.
June 20, 2007 - Day 6
We visited and got an explanation from the doctor....though his words were somewhat encouraging, it was still hard to keep our spirits up. Overall not a great day. I didn't take any pictures, as he was well-sedated and not doing much.
By the end of the day, his volumes had come down somewhat, back to where he had started around 35.
June 19, 2007 - Day 5
The numbers we are most interested in seeing are those that mean he's being weaned off the ECMO machine. They measure the oxygen saturation going into his body, and the same value coming out. The higher the second number, the less Andrew needs the oxygen from the machine, and the more he's producing himself. When that number looks good, then the nurses can lower the flow of blood from the ECMO. When he first went on, the flow number was 36....and the lower the better. During this day, his flow went down to 32 for a while, and even dropped to 30 for a bit. Very encouraging, even though the change was a small percentage of the total.
In the morning, D and I visited....in the afternoon, D's mom and I went in. They were able to remove an IV from his foot, so his lower half looks a lot better....there won't be any upper-half tubes removed for a while.
Jun 21, 2007
Day 4 Pictures
June 18, 2007 - Day 4
In the afternoon I went back with my mom, and Andrew was actually quite active. They keep him well sedated so that he's not in pain and won't move around too much, and they also give him paralytics so that he won't pull out the ECMO tubes....that would be a BAD thing. However, because there's an ebb and flow in his medication and sleep cycles, he is sometimes more or less awake, depending on what time we visit. When we were there in the afternoon, he was moving his leg a bit, taking some breaths, pushing against my mom's hand with his foot, and even trying to open his eyes. The sedation kept him groggy, but it was really nice to see some activity, and to be able to bring home video and pictures of him opening his eyes (just a little).
His vitals stayed normal throughout the day. There's always something that's a little high or a little low, and it's occasionally alarming, but we're starting to get used to the idea that they can regulate these things with the appropriate medication, and one number out of whack is nothing to be alarmed about. It's a time for patience, as we just have to let things happen naturally and let Andrew fight to get better. The ECMO has given him the best opportunity to do so, and we have to let it happen.
June 17, 2007 - Day 3
In the afternoon, I visited with my mom, who was very glad to see him. I think actually being in there with him makes everything a little more "real," especially his recovery. The last anyone but us had seen him, he was still blue....and it really helps to see him pink and cute. Unfortunately, the visitor list is VERY limited and strictly enforced, and we won't be able to put anyone but grandparents on. However, we've told Andrew that he has a huge family that loves him very much, and that we'll have to physically restrain you all from visiting at once when he comes home.
It was nice to see him peaceful and resting, but not much happened with his vitals.
June 16, 2007 - Day 2
We spoke to the doctor and saw some X-rays from before the pneumothorax, after the collapsed lung, and after the chest tube. His right lung looked a lot better after the chest tube, and appeared to fill the entire right side of his chest cavity...a good sign. His 'numbers,' a LONG list of statistics gathered from various electronic monitors and blood tests, were pretty stable, and recovering somewhat from the trauma of his first day of life. We headed back to the hospital so D could continue to recover. She's saving up 'food' for Andrew to eat when he recovers, so we're somewhat limited to three/four hours out in public at a time.
I headed back that evening to check up on the baby. I sat there and talked to him for a while....he can hear us, even though his muscles are being 'paralyzed' and he's sedated to remove any pain. I also took some more pictures. While I sat there, the doctor came by several times and varied the oxygen input to test out better treatments. They also tried moving his head to the other side (on the vent, his head either has to be directly left or directly right). When his blood oxygen saturation started dropping significantly, they even tried rolling him over onto his stomach for a bit.
Eventually, the doctor decided that nothing was working, even on 100% oxygen, a nitric oxide addition, a surfactant treatment, and multiple body positions. [I apologize for the medical jargon...feel free to ignore it, or look these terms up on your own.] The next step after standard ventilator treatments is to put a child on an ECMO machine. ECMO stands for Extra Corporeal Membrane Oxygenation....it's another term for a heart/lung bypass machine for pediatric patients. Children's is the only facility in San Diego County that has these machines, and we were very lucky to be so near for the delivery.
In the NICU, surgeries are done in-place. The surgeon came over from the ER, the surgical team brings in sterile gear, and everybody gowns up and scrubs in for the surgery. I was kicked out of the ward at that point, and had to sit in the waiting room while the surgery was performed. I left the room at 1am and the surgery didn't end until 3:30am. The surgeon came out and described how the procedure went...it took a long time, but Andrew came through well. Putting a child on the bypass means that their heart and lungs don't have to work as hard, so a successful surgery takes a lot of effort off his traumatized lungs. His numbers were almost immediately stabilized.
The positive is that the ECMO machine stabilizes his oxygen levels and allows Andrew's lungs to recover from the pneumothorax, ventilator, and other traumas. The downside is the list of possible complications. First, and most importantly, all the blood traveling through the machine is heparinized, which means it won't clot well. That makes any bleed, especially in the brain, very dangerous for the patient. The surgical and IV sites are also susceptible to these clots. Second, the open wounds can lead to infection, which would deal a distinct setback to his medical progress. There are several other minor complications, but bleeding and infection are the most pressing issues.
Once on ECMO, the desired sequence of events would be a stabilization of lung and heart function followed by the hernia surgery and removal from ECMO. It should give Andrew's lungs a chance to heal, so that he will be strong enough to survive on his own after the surgery.
Day 1 Pictures
Jun 20, 2007
June 15, 2007 - Day 1
I won't bore you with the details of the day, but labor progressed as expected. D got an epidural a bit later than expected, so she got to feel some good, solid contractions....a real taste of natural labor. We spent a lot of time staring at the fetal heart rate and contraction monitors, making sure the epidural was working and seeing how the labor moved forward. For a while we were a bit concerned that the fetal heart rate would drop when a contraction came on, but rolling over and changing positions seemed to provide a temporary solution until the problem later disappeared on its own. The doctor kept checking in on us and our nurse was fantastic.....we were very well taken care of.
We'd always been worried about the need for a possible cesarean, due to my large birth weight, pre-labor ultrasounds that showed a big baby with a bigger head, and the fact that both D and I required C-sections. This was a very real possibility, especially when the nurse determined that the baby was coming down face-up, which makes for a more difficult natural delivery. Fortunately, the nurse has been doing this a long time and managed to get him turned around during the "pushing" phase. D started pushing at 3pm, and delivered at 4:58, only ten hours after arriving. Andrew was delivered, suctioned, snipped (umbilical), and handed over to the nurse.
The first indication we had that anything was wrong was when we didn't hear a cry. The "delivering a baby" scene in TV and movies only has a few main requirements...a "mother pushing" scene, an "I see the head" moment, and a "baby screaming" view. Believe me, D did her share of pushing, and I got a good look at his head on the way out.....but we didn't hear him crying. That was scary enough, but the flood of doctors and nurses that followed was even worse. They performed CPR on him to ensure that his heart was still beating, they tried to "bag" him to give him some air, and eventually they had to intubate in order to get some oxygen in. Everyone seemed a bit stymied initially, but the first possible diagnosis we heard was a pneumothorax, as they weren't hearing any breath sounds from his left side. They wheeled him out of the room and down to the nursery, where they did a chest X-ray and determined the actual problem....the diaphragmatic hernia. The reason they hadn't heard any breath sounds from the left side is because his digestive tract was taking up that space, rather than his lung.
Though the doctors and nurses were surprised by this issue, they were very professional and dealt with it as quickly and efficiently as can be expected. They were giving him as much oxygen as they could, but his underdeveloped lungs couldn't process it very well. He improved from dark purple to a light blue, but was still in critical condition and obviously needed some additional help to breathe. They decided to transfer him to Children's Hospital, which is only a short drive away and one of the primary care centers for this sort of neonatal disease (and many others). The three-person transport team arrived, moved him to a mobile cart, and took him to the ambulance for transfer. We got to see him again before he left, and though he was better than at the delivery, it was probably the most scared we've ever been....he looked very sick, very blue, and very fragile.
D obviously had to stay in recovery, so I drove over to Children's to see how he did after the transfer. I was there for a few hours and spoke both to the transfer team and to the neonatologist that worked on him after he arrived. There was both good news and bad news. The bad news was that a pneumothorax had developed sometime between his first chest X-ray and arriving at Children's for his next X-ray. This meant that his "good" right lung had a hole in it, collapsing his lung and filling his chest cavity with air. They had to put in a chest tube to drain the released oxygen, which was successful, but the collapse didn't bode well for his lungs being able to take over. The good news was that he had actually gotten a little better in the ambulance on the way over, and that he didn't (yet) have to be put on the most advanced life support machines. Even on a normal respirator, he was looking MUCH better than he had been when he left.
The Neonatal ICU at Children's is only for the most critical kids, and Andrew definitely applies. In order to have the best access to give him medicine, draw blood, and provide other care, they inserted multiple IV lines (in his arm, foot, and umbilical cord), a ventilator, a stomach tube, and the aforementioned chest tube. His arms and legs were splayed out to the sides, he was sedated so that he wouldn't feel any pain, and he looked a little doll-like....however, he still looked 100x better than earlier, and I was just happy to see him pink. In the wee hours of the morning, I went back to the hospital and spent the night with D, who was recovering nicely but understandably emotionally distraught.
[I'll introduce pictures as I took them, starting with pictures from that first night. These pics will look better and worse as I write about later days....but I want the opportunity to explain what's in them instead of throwing a ton of pictures up all at once.]
Medical Info
Diaphragmatic hernias always require surgery for repair, but the true danger lies not in the condition itself, but in the lung problems that go along with the defect. The intestines impinge on developing lungs, restricting them from growing to their full potential. Often, the heart and opposite-side lung are also pushed over and malformed. This results in underdeveloped lungs that don't provide enough oxygen to the newborn baby. Mechanical respiration (a ventilator) is almost always needed, and severe cases can also require a heart-lung bypass machine called an ECMO. Andrew's is a severe case and his lungs require significant help. In addition, there are other defects that can appear in syndromes along with this disease, including heart defects, chromosomal abnormalities, and/or kidney damage. Fortunately, it doesn't appear that Andrew has any of these non-lung related issues.
The Intro
We have been overwhelmed by the outpouring of support and love from our family and friends, but have been unable (both emotionally and logistically) to answer every phone call, email, and card. We want to thank everyone for their thoughts and caring, and though we haven't been able to respond, please be assured that we have heard and appreciated them all.
To this point, we have distributed information through just a few sources. We may rely on you further, but I hope to ease your burden by providing regular updates on this blog. I'll post pictures, news, and other information whenever I can...both during this ordeal and throughout his future (healthy) life.